Key Points:
- Genomic research has been central to understanding and combating the SARS-CoV-2 (COVID-19) pandemic.
- Polymerase chain reaction (PCR) is a laboratory technique that uses selective primers to “copy” specific segments of a DNA sequence.
- COVID-19 PCR tests use primers that match a segment of the virus’s genetic material. This allows many copies of that material to be made, which can be used to detect whether or not the virus is present.
- A positive COVID-19 PCR test means that SARS-CoV-2 is present. A negative result could either mean that the sample did not contain any virus or that there is too little viral genetic material in the sample to be detected.
What is PCR?
Polymerase chain reaction (PCR) is a common laboratory technique used in research and clinical practices to amplify, or copy, small segments of genetic material. PCR is sometimes called “molecular photocopying,” and it is incredibly accurate and sensitive. Short sequences called primers are used to selectively amplify a specific DNA sequence. PCR was invented in the 1980s and is now used in a variety of ways, including DNA fingerprinting, diagnosing genetic disorders and detecting bacteria or viruses. Because molecular and genetic analyses require significant amounts of a DNA sample, it is nearly impossible for researchers to study isolated pieces of genetic material without PCR amplification.

How does COVID-19 PCR testing work?
COVID-19 testing uses a modified version of PCR called quantitative polymerase chain reaction (qPCR). This method adds fluorescent dyes to the PCR process to measure the amount of genetic material in a sample. In this instance, healthcare workers measure the amount of genetic material from SARS-CoV-2.
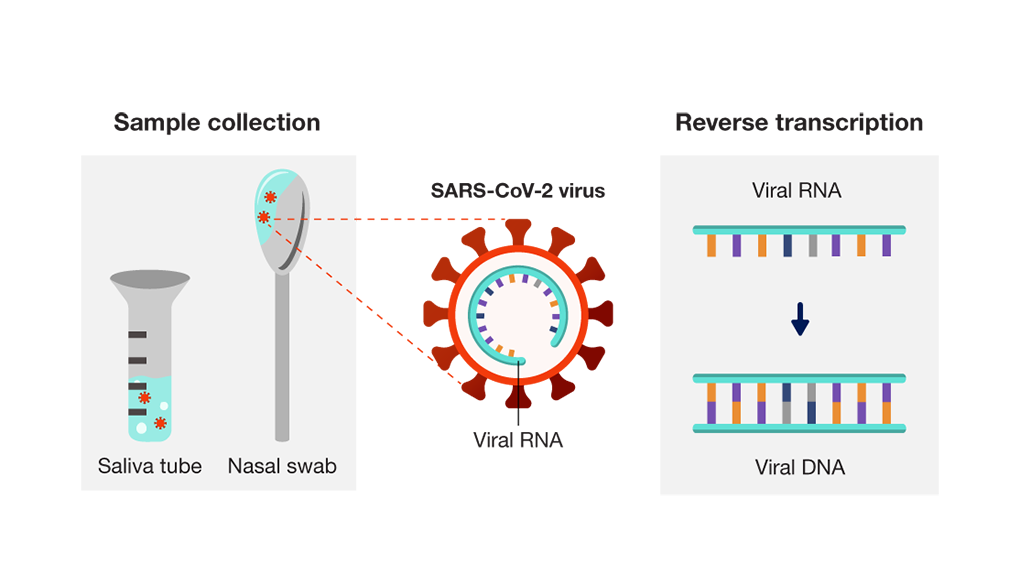
The testing process begins when healthcare workers collect samples using a nasal swab or saliva tube. The SARS-CoV-2 virus, which is the pathogen that causes COVID-19, uses RNA as its genetic material. First, the PCR is converted from single-stranded RNA to double-stranded DNA in a process called reverse transcription. The two DNA template strands are then separated.
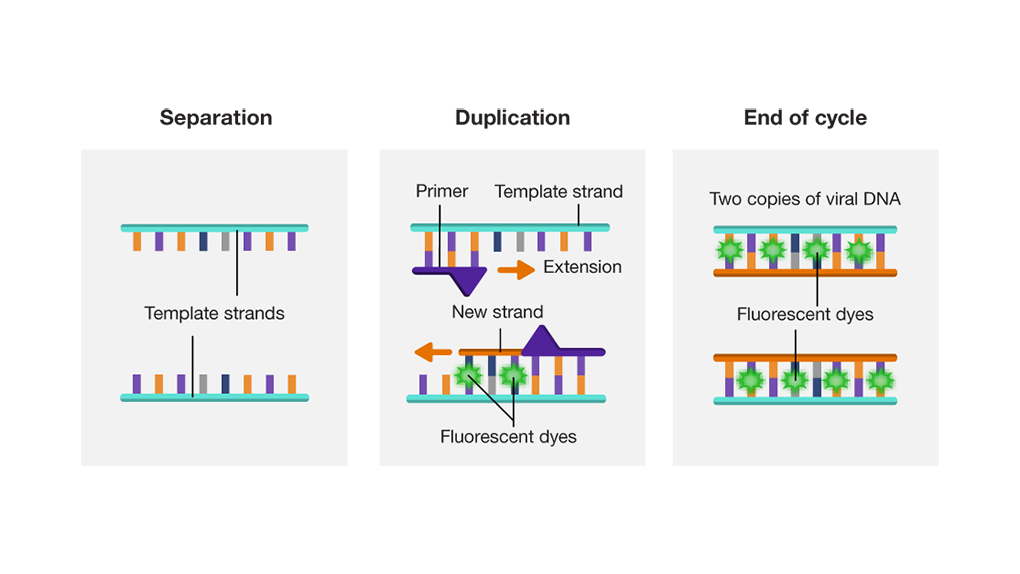
Primers attach to the end of these strands. Primers are small pieces of DNA designed to only connect to a genetic sequence that is specific to the viral DNA, ensuring only viral DNA can be duplicated (right). After the primers attach, new complementary strands of DNA extend along the template strand. As this occurs, fluorescent dyes attach to the DNA, providing a marker of successful duplication. At the end of the process, two identical copies of viral DNA are created. The cycle is then repeated 20-30 times to create hundreds of DNA copies corresponding to the SARS-CoV-2 viral RNA.
What do results mean for a COVID-19 PCR test?
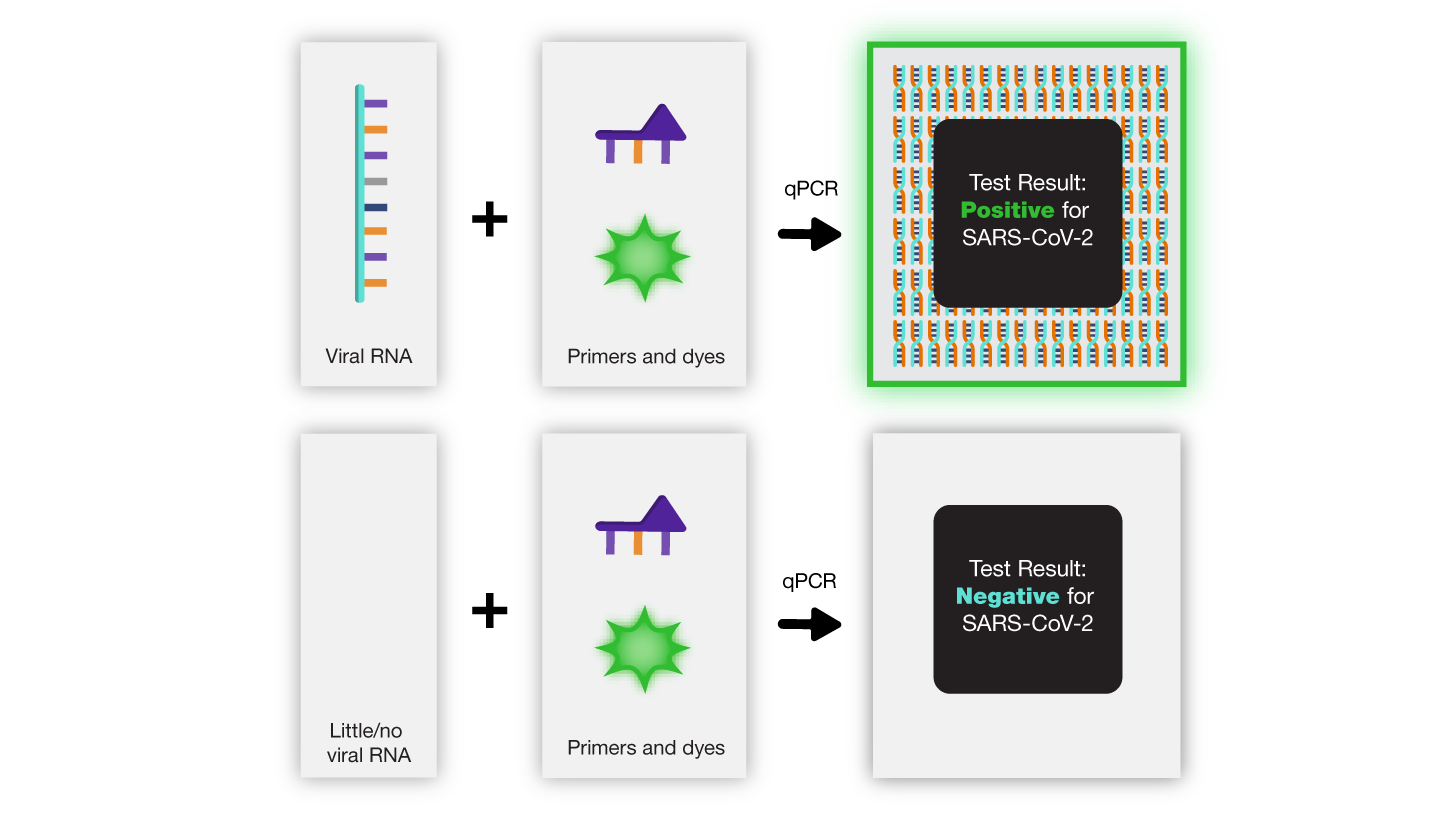
A positive result happens when the SARS-CoV-2 primers match the DNA in the sample and the sequence is amplified, creating millions of copies. This means the sample is from an infected individual. The primers only amplify genetic material from the virus, so it is unlikely a sample will be positive if viral RNA is not present. If it does, it is called a false positive.
A negative result happens when the SARS-CoV-2 primers do not match the genetic material in the sample and there is no amplification. This means the sample did not contain any virus.
A false negative result happens when a person is infected, but there is not enough viral genetic material in the sample for the PCR test to detect it. This can happen early after a person is exposed. Overall, false negative results are much more likely than false positive results.
Last updated: January 18, 2022