Last updated: July 31, 2012
Researchers identify potential treatment for the lethal premature aging disorder progeria
Researchers identify potential treatment for the lethal premature aging disorder progeria
Rapamycin shown to slow cellular aging and reduce accumulation of toxic protein in cells
By Raymond MacDougall
Associate Communications Director for Intramural Research
 |
"This is an exciting new development in our efforts to understand the cellular mechanisms of progeria," said senior author and NIH Director Francis S. Collins, M.D., Ph.D. "Our collaboration on this study is building a momentum of scientific insight that will hopefully contribute therapies for this devastating condition. It also illuminates our fundamental knowledge of aging in cells and organisms."
Progeria is a genetic disorder characterized by dramatic premature aging. Both parents of progeria patients have normal genes, indicating that each child has a new mutation in the affected gene, which is why it is extremely rare. Young children with progeria exhibit features and symptoms of advanced age, including hair loss, diminished subcutaneous fat, premature atherosclerosis and skeletal abnormalities. These children typically die from heart attack or stroke in their teens.
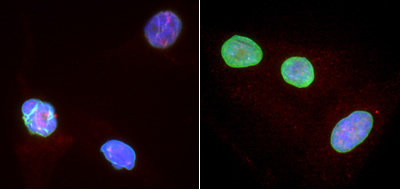
In 2003, NHGRI researchers discovered that progeria is caused by a mutation in the gene for Lamin A. Lamin A is a protein that helps to maintain the normal structure of a cell's nucleus, the cellular repository of genetic information. Progerin, a toxic protein, is produced as a result of a mutation in the Lamin A gene. But recently, progerin has also been found to accumulate, although at a much slower rate, as normal cells age.
In the study, published June 29, 2011 in the early online edition of Science Translational Medicine, researchers treated cells of patients affected by progeria with rapamycin. Rapamycin, currently used to reduce the risk of organ transplant rejection, reversed damage to the cell nucleus seen in progeria, damage caused by an accumulation of the toxic protein progerin inside the cell. The study also showed that rapamycin flushes progerin out of the cell.
Lead author Kan Cao, Ph.D., is an assistant professor of Cell Biology and Molecular Genetics at the University of Maryland, College Park, a position she has held since September 2010. She formerly spent five years as a postdoctoral fellow in the NHGRI Molecular Genetics Section, Genome Technology Branch. In 2009, after reading about a mouse study in which rapamycin extended the normal animals' lifespan, Dr. Cao acted on a hunch and directed a preliminary experiment using the drug to treat progeria cells in culture. Her hunch proved fortuitous: After three weeks, all of the cells treated with rapamycin looked healthier.
Dr. Cao observed that rapamycin affects progeria cells over a number of weeks. She surmised that rapamycin's affect on these cells may be related to cell division. "Progerin collects as large collections of debris in the cytoplasm after mitosis," Dr. Cao said. "Rapamycin helps the clearance of progerin from the cytoplasm. In time, accumulation of progerin is significantly delayed by the affect of rapamycin."
In the current study, the researchers replicated Dr. Cao's experiment using cells from three progeria patients compared with cells from four healthy individuals. They observed that progeria cells treated with rapamycin showed a reversal over time in the structural alterations of the nucleus that occurs with the disorder and that rapamycin treatment helps prevent DNA damage within the nucleus. After 60 days of treatment, the researchers observed a beneficial effect of reduced aging on both normal and progeria cells.
Collaborators in the research from the Mass General Institute for Neurodegenerative Disease, led by co-senior author Dimitri Krainc, M.D., Ph.D., associate professor of neurology at Harvard Medical School, explored the cellular process called autophagy, which is an essential process in the life of a cell where components no longer needed by the cell are broken down. They showed that rapamycin activates a signal pathway that initiates protein degradation, which is part of the autophagy cell process. As for the toxic progerin protein, its level in rapamycin-treated cells declined by half.
"During normal aging our cells accumulate byproducts of normal cell function." Dr. Krainc said. "The ability of cells to remove this debris declines with aging. It is thought that even a small activation of these degradation systems that normally exists in cells would extend the health and lifespan of our cells and organs."
Dr. Krainc explained that one of the effects of rapamycin is to activate debris-degradation systems in cells. "Progerin that causes progeria also accumulates, although in very small amounts, in normal aging," he said. "However, if rapamycin proves to have beneficial effects in lifespan in humans it is safe to assume that it will not be just because it may clear progerin from cells, but also because it clears other toxic products that accumulate during aging."
In a separate study published June 13, 2011 in the Journal of Clinical Investigation, members of this research team showed that progerin is activated in normally aging cells as telomeres, the protective end caps on chromosomes, are degraded.
"This is the beginning of our work," said Dr. Cao. "We want to understand the disease inside and out — from the cellular phenotypes to the molecular mechanisms. We also want to find potential therapies and ways that with new technologies we can use our understanding of progeria as a model system for normal aging."
Based on these results, a clinical trial looking at the effects of rapamycin in children with progeria is currently being explored.
For a photo depicting a child affected by progeria, go to:
http://www.genome.gov/dmd/img.cfm?node=Photos/People/People%20Outside%20NHGRI&id=79252
For more about Hutchinson-Gilford progeria syndrome, go to Learning About Progeria.
